Manuscript accepted on : September 11, 2009
Published online on: 28-12-2009
N.C. Sivakumar2, Indira A. Jayaraj2, R. Jayaraj2 and D. Srinivasa Rao1
2Kongunadu Arts and Science college, Coimbatore, India.
1Center for Biotechnology, Acharya Nagarjuna University, Guntur India.
Corresponding Author E-mail : srine.rao@gmail.com
ABSTRACT: To determine the insulin resistance in PCOS women of rural and urban area, BMI, Fasting glucose and Fasting insulin levels measured in 120 PCOS women (60 from rural and 60 from urban) and 10 normal from rural and urban women were recruited for control. It was found that urban PCOS women had mean BMI of 29±4.3 kg/m2 and rural PCOS women had mean BMI of 27±3.6 kg/m2.The insulin resistance of urban PCOS and rural PCOS women were 8.65±2.9 and 9.85±3.2 kg/m2 respectively. The Urban PCOS women had high BMI and low insulin resistance when compared with the rural PCOS women.
KEYWORDS: Insulin resistance; polycystic ovarian syndrome; rural; urban areas
Download this article as:| Copy the following to cite this article: Sivakumar. N. C, Jayaraj. I. A, Jayaraj. R, Rao. D. S. A Comparative Study of Insulin Resistance in Infertile Women With Polycystic Ovarian Syndrome in the Rural and Urban Areas. Biosci Biotechnol Res Asia 2009;6(2) |
| Copy the following to cite this URL: Sivakumar. N. C, Jayaraj. I. A, Jayaraj. R, Rao. D. S. A Comparative Study of Insulin Resistance in Infertile Women With Polycystic Ovarian Syndrome in the Rural and Urban Areas. Biosci Biotechnol Res Asia 2009;6(2). Available from: https://www.biotech-asia.org/?p=9034 |
Introduction
Polycystic ovarian syndrome (PCOS) is the most common endocrine disease in women of reproductive age and is estimated to affect 7-8 % of the population (1). Polycystic ovarian syndrome is characterized by chronic anovulation and hyperandrogenism. According to revised guidelines of PCOS consensus workshop group, to be diagnosed with PCOS, a woman must have 2 of the following 3 manifestations; irregular or absent ovulation, elevated levels of androgenic hormones and/or enlarged ovaries containing at least 12 follicles each (2). Poly cystic ovaries are defined as those who found on ultrasound to contain 12 or more follicles measuring 2 to 9 mm in diameter and / or have an increased ovarian volume of 10 ml or greater. Only one ovary fulfilling these criteria is enough to meet the definition of poly cystic ovaries. Prominent features of the syndrome include hirsutism, menstrual dysfunction, infertility, elevated androgen levels and insulin resistances. Women with PCOS have a clustering of cardiovascular risk factors, such as obesity, lipid abnormalities, impaired glucose tolerance and hypertension (3).
Reproductive function has been shown to be sensitive to changes in the physical, psychosocial and chemical environments. Although reproductive effectives of occupational exposure to hazardous chemicals have been well documented in the literature, the potential effects of chemical containments at levels representative of contemporary exposure in the general population are much less certain (4). Evidence for adverse effects of exposure to environmental contaminants is more conclusive among the lower animals than for humans where considerable controversy remains. In addition to potential reproductive hazards of exposure to contaminants, there is also evidence for adverse reproductive effects of the physical and psychosocial environments (5).
Insulin resistance is thought to be the uniting pathogenic factor in the associations between hypertension, glucose tolerance and obesity (6). To study the prevalence of insulin resistance in the infertility PCOS women and the effect of physical environment and environmental contamination, a comparative study was done among the infertility women residing in urban and rural areas in and around the Coimbatore city.
Materials and Methods
This was a prospective study done from June 2006 to December 2006 in the Infertility center of Rao Hospital, Coimbatore, Tamilnadu. An ultrasound scan was performed to find out the presence of PCOS in infertile women who came over to the infertility center of Rao Hospital, Coimbatore.
120 infertile women diagnosed to have PCOS by ultrasound scan, 50% of them from urban area and 50% of them rural area were recruited for the study. In these women, fasting blood sample was drawn for detecting glucose and insulin levels. Ten normal woman samples from each group were assayed for fasting blood sugar, Insulin levels and were used as controls. The mean age of PCOS Women from Urban are was 27 years and control group was 26.5 years. The mean age of PCOS women form rural area was 29 years and the control group was 28.
Height and weight of each woman measured and the Body Mass Index (BMI) was calculated by dividing their weight in kilogram by the square meter of their height (kg/m²) (7). The women were divided into three BMI groups based on ACOG criteria; normal BMI < 25 kg/ m2; over weight 25-30 kg/m2; and obese > 30 kg/m2 . Fasting plasma glucose was estimated by GOD – POD method (8). Insulin level was measured by Enzyme – Linked Immunosorbant Assay (ELISA) according to the procedure described by Anderson et al., 1993.
Statistical Analysis
All data were expressed as mean ± SD. Comparison among continuous variables was done by student “t” test. A “P Value <0.05 was considered statistically significant.
Results and Discussion
The association between hyperinsulinemia and PCO was first noted by Scarpitta and Sinagra (2000) (9), who found a significant positive correlation between insulin among PCOS women. Obesity and insulin resistance are frequently encounted features PCOS.The present study was aimed to determine the correlation between age, obesity, fasting blood sugar and fasting insulin levels and the results are debited in tables 1, 2 and 3. Figure –1 debits ultra- sonographic image of normal and poly cystic ovary.
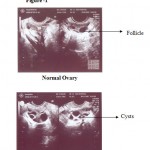 |
Figure 1
|
Table 1: Comparison of Insulin Resistance with PCO and Normal women.
| Parameters | Interfile women (urban) |
Infertile women (rural)
|
||
| PCOS (n = 60) | Normal
(n = 10) |
PCOS (n = 60) | Normal (n = 10) | |
| Age (years) | 27 +3.6** | 26.5+4.0** | 29+4.5** | 28.1+3.2** |
| BMI (kg/m2) | 29.7+ 4.3* | 22.1+3.0* | 27+3.6* | 23.2+2.0* |
| Fasting Glucose (mg/dl) | 90. 9 +9.0** | 86+7.2** | 85.7+6.3** | 81+ 6.9** |
| Fasting Insulin(miu/ml) | 10.5 ± 1.6* | 5.4 ± 0.9* | 8.7 ± 1.3* | 4.5 ± 0.5* |
| Glucose/Insulin ratio | 8.65 ±1.3* | 15.9±1.8* | 9.85 ± 1.4* | 18.0± 1.9* |
Values are expressed by mean ± SD of ` n’ no. of patients.
Means followed by a common superscript * are significant. Means followed by a common superscript ** are not significant.
Groups compared: BMI Vs Fasting blood sugar, BMI Vs Fasting Insulin and FBS/Insulin ratio.
Age Vs Fasting blood sugar, Age Vs Fasting Insulin and FBS/Insulin ratio.
Satistical comparison : P < 0.05
Table: 2. Insulin Resistance in Urban area women (n=60 )
| S. No. | BMI Group
|
No.of patients | Fasting blood sugar mg/dl (Mean ± SD) | Fasting insulin miu/ml
(Mean ± SD) |
Fasting blood sugar/ insulin ratio (Mean ± SD) |
| 1. | Normal (< 25kg/m2) | 20 | 77 ± 2.7** | 6.3 ± 0.5 * | 12.2 ± 0.9* |
| 2. | High (25-30kg/m2) | 24 | 94 ± 3.6** | 8.1 ± 0.6 * | 11.6 ± 0.7* |
| 3. | Obese (> 30 kg/m2) | 16 | 105 ± 4.5** | 17.1 ± 1.5 * | 6.1 ± 0.4 * |
Values are expressed by mean ± SD of no. of patients.
Means followed by a common superscript * are significant. Means followed by a common superscript ** are not significant.
Groups compared : BMI Vs Fasting blood sugar, BMI Vs Fasting Insulin, FBS/Insulin ratio.
Statistical comparison : P < 0.05
Table: 3. Insulin Resistance in Rural area women (n=60 )
| S. No. | BMI Group | No.of patients | Fasting blood sugar mg/dl (Mean ± SD) | Fasting insulin miu/ml
(Mean ± SD) |
Fasting blood sugar/ insulin ratio (Mean ± SD) |
| 1. | Normal (< 25kg/m2) | 30 | 72 ± 2.5** | 5.4 ± 0.4 * | 13.3 ± 1.2* |
| 2. | High (25-30kg/m2) | 16 | 86 ± 3.3** | 7.0 ± 0.8* | 12.2 ± 1.0* |
| 3. | Obese (> 30 kg/m2) | 14 | 99 ± 4.1** | 15.3 ± 1.6* | 6.4 ± 0.7* |
Values are expressed by mean ± SD of no. of patients.
Means followed by a common superscript * are significant. Means followed by a common superscript ** are not significant.
Groups compared : BMI Vs Fasting blood sugar, BMI Vs Fasting Insulin, FBS/Insulin ratio.
Statistical comparison : P < 0.05
The relationship among obesity, fasting blood sugar and hyperinsulinemia, in 60 PCOS women from urban area, we found that 20 had normal BMI, 24 with high and 16 were obese. Among 60 PCOS women from rural area 30 had normal BMI, 16 with high BMI and 14 were obese. The average value of fasting blood sugar for urban and rural women with PCOS was 90.9 mg/dl and 85.7 mg/dl and for the normal groups it was 86 and 81mg/dl to the rural and urban areas respectively.
Insulin resistance (Fasting blood sugar / Fasting Insulin ratio) was calculated and found to be 8.65 and 15.9 in PCOS of the normal women. The Insulin resistance in rural PCOS women was 9.85 and for normal woman it was 18.
This study was attempted mainly to understand the interrelationship between insulin resistance and BMI and the prevalence’s of PCOS in urban and rural women. We found a significant increase in BMI in urban area women when compared to rural area women. That might be due to mechanization of jobs and transportation, availability of processed and fast foods, dependence on television for leisure, less physically active lifestyles and consuming more “energy – dense, nutrient – poor” diets (10). These changes have been an impact on dietary practices and the levels of physical- activity, which causes obesity. Obesity has serious long – term consequences. It can contribute to many problems in women’s reproductive system like prolonged or heavy periods, menstrual pain, delayed ovulation, mid cycle spotting, short luteal phase, premenstrual spotting, infertility, amenorrhea, fibroids, tumors of uterus, breast cancer, endometrial cancer, ovarian cancer, uterine prolapse etc.(11) .
In a recent study among women in northern Indian by Agrwal and Mishra (2004) (12), it was found that urban residence significantly increase the risk of obesity. The transition from a rural to an urban life styles is associated with increased levels of obesity, which has been linked with dramatic changes in lifestyles. Urban residence and higher income were associated with higher fat intake, and lower physical activity level compared to rural residence (13). Further the growing popularity of taking fast food is strongly associated with higher BMI brought about by globalization (14). It is well documented that the correlation of insulin resistance and the prevalence of PCOS in women. Further, insulin resistance can be influenced by age and obesity, which are also considered as an important dependent causes of insulin resistance. High BMI is not only associated with increased fasting blood sugar and insulin resistance but also affect the reproductive health of women, by forming PCOS.
Conclusion
Urban PCOS women had high BMI and low insulin resistance than rural PCOS. We therefore conclude that urban occupational exposures and life style changes with less physical work might be the reason for high BMI with low insulin resistance and decreased fertility in urban women than rural women.
References
- Dasgupta, S. and Reddy, B.M. Present status of understanding on the genetic etiology of polycystic ovary syndrome. Postgrad. Med. 54: 115-25 (2008).
- Rotterdam (2004). ESHRE/ASRM – Sponsored PCOS Consensus Workshop group. Revised 2003 consensus on diagnostic criteria and long- term health risks related to poly cystic ovarian syndrome. Ster. 81:.94 – 25 (2004).
- Pasquali R and A Gambineri. Poly cystic ovary syndrome:a multifaceted disease from adolescence to adult age. N.Y. Acad. Sci. 1092:158-74 (2006).
- D., Cifkova.R., Fanta.M., Poledne.R., Zinvy. J and Skibova.J. Increased risk of non-insulin dependent diabetes mellitus, arterial hypertension and coronary artery disease in pre menopausal women with a history of the poly cystic ovary syndrome. Hum. Reprod. 15(4): 785-786 (2000).
- Younglai E.V., Holloway A.C. and Foster W.G. Environmental and occu-pational factors affecting fertility and IVF success. Reprod.Update.11:43 – 57(2005).
- , Essah P.A., Inorno M.J. and Nestler J.E. Prevalence and Characteristics of the metabolic syndrome in women with polycystic ovary syndrome J. Clin. Endocrinal. Metab. 90 : 1929 – 35 (2005).
- Triuder P. Clin. Biochem. 6 : 24-25 (1969)
- G.A., Willet W.C., Ronitzkey, A. and Manson J.E. Weight gain as a risk factor for clinical diabetes mellitus in Women. Ann. Inter med. 122: 481 – 486(1995).
- Anderson L., Dinesen .B., Jorgenson P.N., Poulsen F and Roder M.F. Enzyme immunoassay for intact human insulin in serum. Chem. 38 : 578 – 582 (1993).
- A.M., and Sinagra D. Poly cystic ovarian syndrome an endocrine and metabolic disease. Gynecol. Endocrinol 14 : 392-5 (2000).
- Shannon M. ‘An emphathetic look at overweight’,CCL Family Foundations. 20:3-4 (1993).
- Agrawal P. and Mishra V.Covariates of overweight and obesity among women in North India. East West center working paper, Population and Health Series, No. January (2004).
- Sobngwi E., Mbanya.J.C., Unwin N.C., Kengne L., Fezeu E.M., Minkonlou T.L., Aspray and Alberti K.G.(2002). Physical activity and its relationship with obesity hypertension and diabetes in urban and rural Cameroon, International Journal of Obesity and Related Metabolic Disorder 26 :1009-16 (2002).
- Scholsser, E. Fast Food Nation. The dark side of American meal (2002).

This work is licensed under a Creative Commons Attribution 4.0 International License.





